P&C Insurance Software Solutions

Policy Management
Easily manage your insurance policies with Practo Insura. From billing to claims and document handling, our integrated system covers all aspects of your policies, putting everything you need right at your fingertips.
About Policy Administration
Insured Portal
Enhance customer engagement with our customizable policyholder portal. As part of our Policy Administration Suite, this feature creates a better experience for everyone, helping to build stronger relationships and keeping everyone informed and valued throughout their insurance journey.
About Insured Portal
Insurance Strategy Consulting
Strategic consulting services for insurers, MGAs, and reinsurers - focused on Go to Market planning, risk and capital structuring, Insurtech transformation, and U.S. regulatory compliance. Designed to help you drive growth, ensure compliance, and improve operational performance.
About Consulting Services
AI Agents For Insurance
AI Voice & Chat Agents are purpose-built for insurers to automate first-level support like FNOL, quotes, billing, and renewals 24/7 across voice and chat. They reduce operational load, lower AHT, and enhance CX while staying fully compliant. The platform supports multilingual interactions, integrates with core systems.
About AI Support AgentsWhy Choose Practo Insura?
Rapid Rater Algorithm
Why wait 2 months to update insurance rates? With Practo Insura, new rates can be implemented & made live in just 7 days. Our advanced rater system ensures swift and accurate updates including premium, fees & coverage factors, keeping you ahead of the competition and dynamic to market changes.
Policy Data Migration
Worried about switching to a new system? We’ve got you covered. Our data migration feature ensures you can pick up exactly where you left off without waiting 6 months on old system. If you’ve got a properly structured policy dataset, you can instantly switch your system with Practo Insura, so there’s no interruption to your operations.
Custom E-Sign Tool
Say goodbye to paper-heavy processes! Our built-in e-signature tool is designed to make policy agreements hassle-free and secure. Whether you're finalizing new policies or updating existing ones, our tool saves you time and simplifies workflows.
User-Friendly Design
We believe technology should simplify life, not complicate it. That’s why our software is designed with user experience at its heart-intuitive, simple, and accessible for everyone.
Paperless Process
Join us in embracing a greener future. Our paperless processes not only streamline your operations but also contribute to environmental sustainability.
Strategic Partnership
When you choose Practo Insura, you gain more than a software provider-you gain a partner who is committed to your success. We grow with you, ensuring our solutions evolve with your changing needs.
What Our Clients Say
Delivering P&C Insurance Carrier Solutions Since 2016
Practo Insura Insights
Why Claims Data Matters in Product Design for U.S. P&C Insurer
Claims data has traditionally been treated as a record of past losses, used mainly for reserving, reporting, and post-event analysis. But in today's U.S. P&C market, where repair severity, litigation exposure, climate volatility, and emerging risks are changing faster than traditional product cycles, claims data is becoming a strategic input for product design, pricing, and underwriting decisions.
The real challenge is no longer whether insurers have claims data, every carrier does. The challenge is how quickly they can convert claims signals into business action. As the gap between changing risk conditions and organizational response widens, claims intelligence is becoming a critical capability for improving underwriting performance, product relevance, and long-term profitability.
What is Detection Gap in Modern Insurance Product Design
Most carriers do not struggle because they lack claims data. They struggle because there is often a significant gap between when a claims trend emerges and when the organization takes action.
Consider a common auto insurance example. Claims teams may start seeing higher repair severity for specific vehicle segments due to increasing ADAS calibration requirements, longer repair cycles, or more expensive replacement parts. The signal exists. The data exists. The problem is that product, underwriting, and pricing teams may not see that trend until months later through formal reviews or profitability reporting.
That delay creates what can be called the Detection Gap, the period between when claims data first signals a meaningful change in risk and when the organization responds with a pricing, underwriting, or product adjustment.
Why the Detection Gap Matters
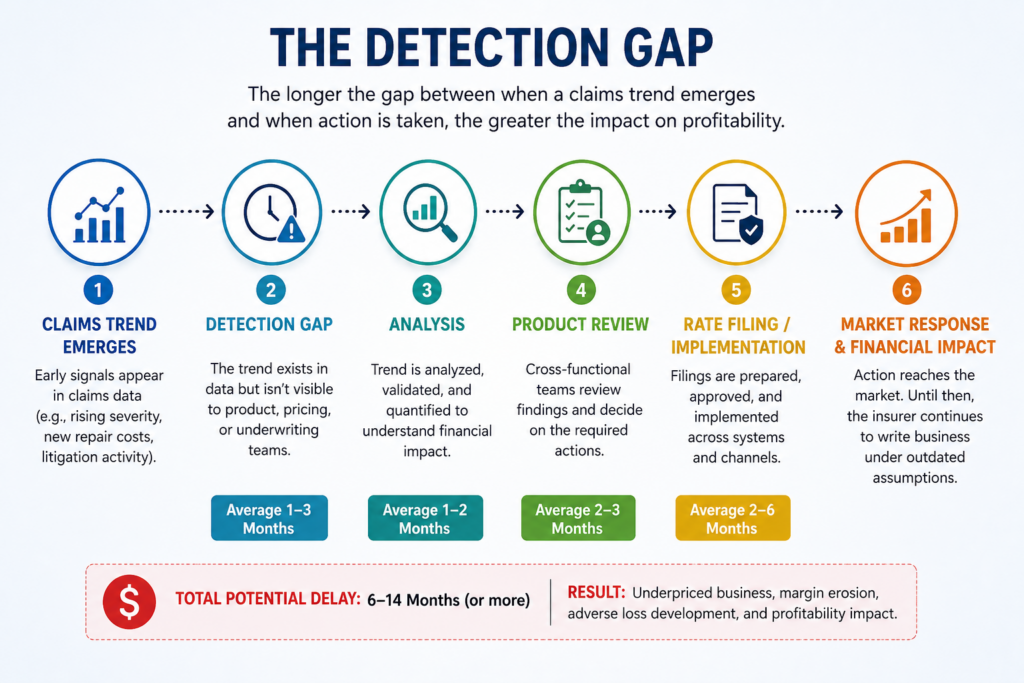
The financial impact of a claims trend is rarely immediate. Instead, it accumulates quietly across hundreds or thousands of policies before it becomes visible in portfolio-level metrics.
- A severity trend may emerge today.
- A product team may detect it three months later.
- Analysis and validation may take another two months.
- A rate filing may require several more months before implementation.
By the time corrective action reaches the market, an insurer may have spent nearly a year writing business under assumptions that no longer reflect actual risk conditions.
The challenge is not limited to auto insurance. Similar detection gaps appear across P&C lines through:
- emerging weather-related loss patterns
- litigation-driven bodily injury severity
- coverage disputes and claims escalation trends
- organized fraud activity
- geographic concentration risk
In many cases, claims activity identifies these issues long before they appear in underwriting profitability reports.
From Claims Data to Business Action
Closing the detection gap requires insurers to think differently about claims information.
Claims data alone has limited value. What matters is how quickly that data becomes actionable intelligence.
The progression looks like this:
Claims Data → Pattern Detection → Business Decision → Product Action
The faster an organization moves through this cycle, the faster it can:
- adjust pricing assumptions
- refine underwriting appetite
- redesign coverage structures
- manage emerging risks
- protect portfolio profitability
This is why leading insurers increasingly treat claims intelligence as a strategic product management capability rather than a claims reporting function.
Why Claims Data Has Become a Strategic Product Asset
Claims data was once treated mainly as an operational record: what happened, what was paid, and how claims were handled. But for modern P&C insurers, that view is too limited.
Every product decision eventually shows up in claims. Pricing decisions affect profitability. Underwriting rules affect loss frequency. Coverage wording affects disputes. Deductibles affect claim behavior. Geographic expansion affects concentration risk.
That is why claims data has become a strategic product asset. It helps insurers validate whether product assumptions still match real-world risk conditions before problems appear in high-level profitability reports.
For carriers, MGAs, and reinsurers, the value is not simply having more claims data. The value is converting claims signals into faster pricing, underwriting, coverage, and portfolio decisions.
1. Validating Pricing and Underwriting Decisions
Pricing and underwriting decisions are built on assumptions. Claims data is where those assumptions are tested against actual loss behavior.
A rate plan may assume that a certain vehicle class, territory, driver profile, or coverage type carries a predictable level of risk. But once claims begin developing, insurers can see whether that assumption still holds. This is especially important in auto insurance, where repair severity, bodily injury trends, litigation involvement, and vehicle technology can change the economics of a segment quickly.
The impact is already visible in repair data. According to industry research, the average total cost of repair has increased 96.4% since 2009, rising from approximately $2,405 to more than $4,720 in 2024. Nearly half of that increase occurred within the last five years alone. ADAS-related costs are a major contributor. Calibration fees increased from $168 in 2017 to $488 in 2024, while diagnostic-related costs per 100 claims grew from roughly $580 to more than $21,300.
At the same time, auto insurance claims have increased 14% since 2020, while claims severity has risen 36%. For product and underwriting teams, these trends demonstrate how quickly actual loss costs can diverge from historical pricing assumptions.
What Claims Data Helps Validate
Claims data can show whether:
- certain vehicle types are producing higher severity than expected
- specific territories are generating more frequent or more expensive claims
- bodily injury trends are worsening in particular states
- deductible structures still make sense for current repair costs
- underwriting rules are attracting the right risk profile
- rating variables are still aligned with actual loss outcomes
For example, if newer vehicles with advanced safety systems are consistently producing higher repair costs than expected, the issue is not just claims severity. It may indicate that the current pricing model, deductible design, or underwriting assumptions need to be refined.
What Insurers Can Do With This Insight
Product and underwriting teams can use claims intelligence to make targeted changes, such as:
- revising rating factors
- adjusting deductible options
- tightening eligibility rules
- updating underwriting guidelines
- modifying territory assumptions
- flagging specific segments for pricing review
- redesigning coverage structures where loss behavior has changed
This prevents claims insight from staying trapped inside claims operations. It turns the data into a practical input for product and underwriting decisions.
The Result
When insurers use claims data to validate pricing and underwriting assumptions, they gain a clearer view of where the product is still working and where it is drifting away from real risk.
The result is sharper segmentation, better risk selection, stronger rate adequacy, and more disciplined portfolio management.
Related Read: How Insurers Use Predictive Analytics to Improve Underwriting and Risk
2. IdentifyingCoverage Gaps and Emerging Risks
Claims activity often reveals a different kind of product problem: not whether the price is right, but whether the coverage itself still works in the real world.
A product may be priced correctly and still create friction if policy wording is unclear, endorsements are outdated, limits no longer reflect current costs, or new exposures were not considered when the product was designed. These issues usually surface during claims, when customers test the product under actual loss conditions.
What Claims Data Reveals
Claims data can show:
- which coverages generate the most disputes
- where policy language creates confusion
- which endorsements are producing unexpected loss behavior
- whether limits or deductibles still match current repair and replacement costs
- where new risks, such as EV repairs, severe weather, or litigation trends, are creating product pressure
For example, an auto insurer may find that rental reimbursement limits are no longer adequate because repair cycle times have increased. A property insurer may see repeated disputes around water damage or storm-related exclusions. An MGA may discover that a niche endorsement is being used differently than originally expected.
What Insurers Can Do With This Insight
Product teams should treat these patterns as design feedback, not just claims friction.
That means insurers can:
- review dispute trends by coverage type
- analyze escalation patterns tied to specific policy wording
- reassess limits, deductibles, and exclusions against current claim realities
- update endorsements where loss behavior has changed
- involve claims and compliance teams before product changes are finalized
The Result
Using claims data this way helps insurers close coverage gaps before they become larger profitability, litigation, or customer experience problems.
It also makes product design more grounded in real claim behavior, not just market assumptions, competitor forms, or historical coverage structures.
3. Reducing Fraud and Claims Leakage
Fraud is not always obvious at the individual claim level. One inflated repair supplement, one represented injury claim, or one unusual billing pattern may look isolated. The real signal appears when similar patterns repeat across vendors, geographies, coverages, or claim types.
That is where claims intelligence becomes valuable. It helps insurers move beyond claim-by-claim review and identify leakage patterns that point to broader product or process vulnerabilities.
A 2024 study by CLARA Analytics found that AI-driven cohort modeling identified potential fraud indicators within two weeks of claim submission. Approximately 9% of open claims were flagged as strong SIU referral candidates, with the model identifying suspicious activity at a rate comparable to experienced adjusters but significantly earlier in the claim lifecycle.
Where Leakage Often Shows Up
Common signals include:
- repeated supplement requests from specific repair vendors
- abnormal medical billing patterns
- recurring use of the same coverage provisions
- staged accident indicators
- unusual claim timing or clustering
- claim types with higher-than-expected escalation rates
For example, if a specific endorsement is repeatedly involved in questionable claims, the issue may not be limited to fraud investigation. The endorsement itself may need clearer eligibility rules, stronger documentation requirements, or tighter claim controls.
How Insurers Can Respond
Insurers can reduce leakage by:
- standardizing vendor and provider tracking
- connecting SIU findings with product and underwriting teams
- reviewing claim pathways that are repeatedly exploited
- tightening documentation requirements where abuse patterns appear
- monitoring fraud indicators by coverage, vendor, geography, and claim type
Result
This helps insurers reduce avoidable claim costs while improving product discipline.
More importantly, it turns fraud detection into a product feedback mechanism. If claims data shows where the product is being exploited, insurers can redesign the exposure instead of only investigating it after the loss occurs.
Related Read: 5 Questions Every Carrier Must Ask Before Launching a New Line of Business
4. Improving Product Profitability and Portfolio Performance
Growth can hide weakness in a P&C portfolio. A product may continue adding premium while certain geographies, coverages, or customer segments quietly produce more volatility than expected.
Claims intelligence helps insurers separate healthy growth from fragile growth.
According to AM Best, the P&C industry's combined ratio improved from 101.6 in 2023 to 96.6 in 2024, driven in part by stronger pricing discipline, improved underwriting performance, and broader use of analytics.
Where Portfolio Pressure Often Appears
Claims data can reveal:
- geographies with concentrated or worsening loss activity
- coverages creating unexpected volatility
- segments requiring stronger reserve attention
- claim types affecting reinsurance confidence
- products where growth is outpacing risk control
- business classes producing unstable loss development
For example, a carrier may expand successfully in written premium, but claims activity may show that one region is becoming more exposed to weather losses or litigation-heavy claim behavior. That does not always mean the product should exit the market. It may mean the insurer needs tighter appetite rules, different deductibles, revised limits, or a different reinsurance view.
How Insurers Can Respond
Product, underwriting, and portfolio teams can use claims intelligence to:
- identify where growth should be accelerated, slowed, or restricted
- evaluate product performance below the portfolio-average level
- reassess limits, deductibles, and appetite by region or segment
- use claim volatility trends in reinsurance planning
- decide whether certain products need redesign before expansion continues
Result
Claims-informed portfolio management helps insurers grow with more discipline.
It gives leadership a clearer view of which parts of the portfolio are sustainable, which require correction, and which may create future volatility if left unmanaged.
5. Accelerating Product Innovation and Customer Experience Improvements
Product innovation does not always start with a new idea. Sometimes it starts with repeated claims patterns that show where customers need better protection, clearer service, or a product built for newer risk behavior.
Claims data gives insurers a practical view of how products perform after purchase, when the policyholder actually needs the coverage.
In 2024, more than 21 million U.S. policyholders shared telematics data with their insurer, a 28% compound annual growth rate since 2018. Carriers that connected telematics data to actual claims outcomes rather than just pricing models reported up to eight points of combined operating ratio improvement purely from the use of telematics data in claims.
Where Innovation Signals Appear
Claims activity can reveal:
- new protection needs that current products do not address
- claim journeys that create avoidable friction
- service gaps around repair, replacement, or settlement
- opportunities for specialized endorsements
- areas where digital claims support could improve the experience
- risk behaviors that may support usage-based or behavior-based products
For example, recurring EV repair complexity may support a more specialized auto product. Repeated delays in repair coordination may point to the need for stronger repair network partnerships or better digital claims updates.
How Insurers Can Respond
Product and innovation teams can use claims intelligence to:
- validate new product ideas with actual loss experience
- design endorsements around real customer needs
- improve claims communication and service workflows
- modernize products around EVs, telematics, embedded insurance, or usage-based models
- connect claims insights with customer retention and renewal strategy
Result
Claims-informed innovation helps insurers move beyond competitor-driven product development.
It gives them a clearer way to modernize products based on real policyholder behavior, actual loss outcomes, and service friction that directly affects customer trust.
Related Read: 5 Types Usage-Based Auto Insurance
Which Claims Signals Actually Require Product Action?
This section is important because one of the biggest challenges for carriers is not a lack of claims data. It is knowing which signals deserve action and which are simply noise.
Not every increase in claim activity requires a pricing change, product redesign, or underwriting adjustment. The most effective insurers focus on signals that indicate a structural change in risk, profitability, or customer behavior.
High-Priority Signals
These are signals that should typically trigger product, pricing, or underwriting review.
- Significant Severity Increases: When claim severity rises consistently within a specific segment, geography, or coverage type, it may indicate that pricing, deductibles, or underwriting assumptions are no longer aligned with actual loss costs.
- Recurring Coverage Disputes: A growing volume of disputes tied to the same policy provision often signals a product design issue rather than an isolated claims problem.
- Emerging Geographic Concentration: Rising claims activity in a specific region may indicate changing weather patterns, theft trends, litigation exposure, or other evolving risks that require product attention.
- Shifts in Litigation Activity: Changes in attorney involvement, bodily injury severity, or settlement patterns can quickly alter the economics of a product.
Medium-Priority Signals
These signals deserve monitoring but may not immediately require action.
- Temporary Frequency Fluctuations: Short-term spikes caused by seasonality, weather events, or unusual market conditions should be validated before product changes are made.
- Localized Vendor Performance Issues: Problems tied to a specific repair network, contractor, or service provider may require operational intervention before product intervention.
- One-Time Regulatory or Market Events: Certain events may temporarily influence claims outcomes without creating long-term product implications.
Low-Priority Signals
Some claims trends create visibility but rarely justify immediate product action on their own.
Examples include:
- isolated large losses
- individual fraud cases
- short-term claim anomalies
- single-event severity spikes
These events should be monitored but not automatically drive product decisions.
The Goal Is Prioritization
The objective is not to react to every claims trend. It is to identify the signals most likely to affect pricing adequacy, underwriting performance, coverage effectiveness, or portfolio sustainability.
Insurers that establish clear decision triggers can respond more consistently and avoid both overreacting to noise and underreacting to meaningful change.
Conclusion
Claims data is no longer just a record of past losses. It is becoming a product strategy asset for insurers that want to understand how risk is changing in real time.
The real advantage is not having claims data, every carrier has it. The advantage comes from detecting meaningful signals faster and turning them into product, pricing, and underwriting decisions before issues affect profitability or portfolio performance.
As an insurance strategic consultant, Practo Insura helps carriers, MGAs, and reinsurers connect claims intelligence with product strategy, underwriting discipline, and modernization initiatives, helping them build more adaptive products for changing risk conditions.
What Is Subscription Auto Insurance and How to Build It for P&C Insurer in USA
Auto insurance was designed for a market built on long-term vehicle ownership, predictable driving habits, and fixed policy terms.
But mobility is changing. Consumers now expect simpler billing, faster servicing, and models that align with how they access and use vehicles. As subscription-based experiences expand across industries, insurance is also beginning to shift from a rigid annual product to a more adaptable, service-led model.
That is where subscription auto insurance is gaining relevance. It gives insurers a way to align coverage with modern mobility expectations while offering customers a more flexible and convenient experience.
Understanding Subscription Auto Insurance
Subscription auto insurance is more than a shorter policy term. It is a different way of offering coverage.
Instead of putting customers into a fixed 6- or 12-month contract, this model usually works on a monthly recurring basis. Customers pay a flat monthly amount, coverage renews automatically, and changes like cancellation, upgrades, or vehicle swaps are meant to be much easier to handle.
What makes this model different is the way it is structured. Traditional auto insurance is built around a one-time policy purchase that is reviewed later at renewal. Subscription insurance is structured as a continuously active coverage model rather than a fixed-term contract.
It can be offered in two main ways:
- as a standalone monthly insurance product
- as part of a larger mobility package
That larger package may include:
- vehicle access
- maintenance
- roadside assistance
- insurance coverage under one monthly payment
This changes the role of insurance. Instead of being a separate product customers buy on its own, it becomes part of a broader mobility experience.
This also sets it apart from PAYG and PHYD models. PAYG is based on how much a person drives. PHYD is based on how a person drives. Subscription auto insurance is different because it is built around flexibility, simplicity, and convenience, not mileage tracking or behavioral scoring.
So, subscription auto insurance is not just a pricing change. It is a product and distribution model that makes coverage easier to package, manage, and deliver in a more service-driven way.
How Subscription Auto Insurance Works
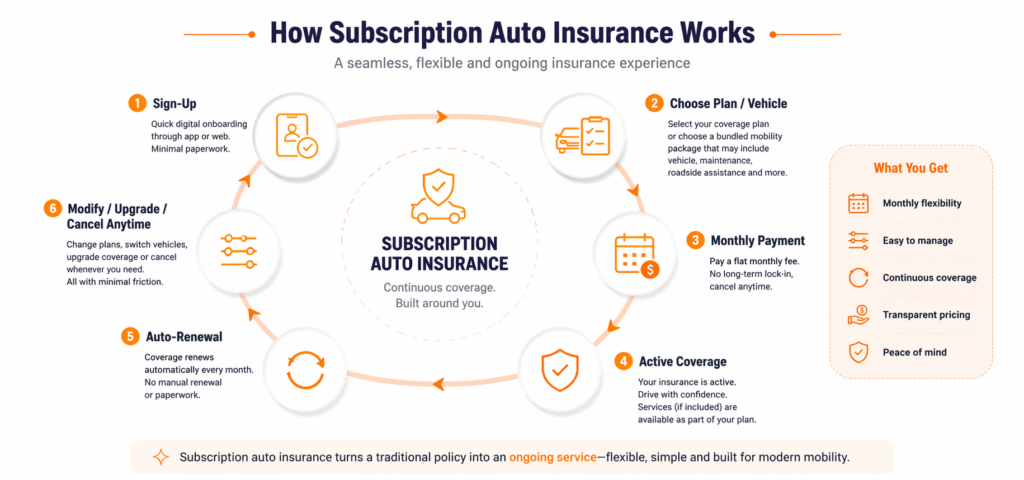
Subscription auto insurance is designed to make coverage easier to start, manage, and continue.
In most cases, the journey begins digitally. Customers sign up online, choose a vehicle or coverage plan, and pay a flat monthly fee. Once activated, coverage renews automatically each month unless the customer decides to change or cancel it.
A typical customer journey looks like this:
- sign up through an app or website
- choose a vehicle, coverage tier, or bundled plan
- pay a monthly subscription fee
- start coverage immediately or on the selected date
- renew automatically each month
- upgrade, switch, or cancel with minimal friction
This makes the experience feel simpler than a traditional auto policy. Instead of managing a long-term insurance contract, the customer interacts with coverage as an ongoing monthly service.
How to Design a Subscription Pricing Model That Works
Pricing subscription auto insurance is not just about setting a monthly fee. The real challenge is designing a model that feels simple and predictable for customers, while still being financially sustainable for the insurer.
Unlike traditional policies, you are not pricing a fixed-term contract. You are pricing an ongoing relationship where customers can change plans, vehicles, and coverage more frequently. That makes pricing more sensitive to churn, duration, and usage patterns over time.
Core Pricing Models Used in Subscription Insurance
| Pricing Approach | How it Works | Best for | Main Advantage | Main Risk |
|---|---|---|---|---|
| Flat monthly pricing | One recurring fee for a standard coverage package | Simple direct-to-consumer offerings | Easy to understand and market | Can underprice risk if segmentation is weak |
| Tiered subscription plans | Multiple monthly plans based on coverage/service level | Insurers wanting flexibility without too much complexity | Supports upsell and clearer customer choice | Requires careful product design across tiers |
| Bundled pricing | Insurance included with vehicle/services in one fee | OEM, car subscription, mobility partnerships | Strong convenience and embedded distribution | Margin visibility and partner cost allocation can get difficult |
What Insurers Must Build Beneath the Monthly Price
Even if the monthly price looks simple to the customer, the pricing logic underneath needs to be carefully structured.
- Base monthly premium logic: Define the recurring price based on coverage level, vehicle category, and target segment. It should be built for a subscription model, not created by simply splitting an annual premium into 12 parts.
- Risk segmentation: Adjust pricing internally using factors like driver profile, geography, and vehicle type. This keeps pricing disciplined without making the customer experience feel complex.
- Bundle cost allocation: Separate the insurance portion from vehicle access or other bundled services. This is important for understanding true margins and avoiding hidden profitability issues.
- Mid-cycle pricing rules Set clear logic for vehicle swaps, plan upgrades, downgrades, or coverage changes during the subscription period. These changes should be handled smoothly without unnecessary friction.
- Proration logic: Calculate fair charges when customers make changes mid-month. This helps maintain billing accuracy while reducing revenue leakage.
Designing Pricing for Flexibility (Where Most Models Fail)
Subscription models break down when pricing cannot adapt to real-world behavior.
Your pricing design must support:
- frequent customer changes without manual intervention
- real-time or near real-time plan adjustments
- consistent billing despite mid-cycle modifications
- smooth transitions between plans or vehicles
If these are not built into pricing logic, operational friction quickly erodes the customer experience.
How to Evaluate Pricing Performance
Subscription auto insurance cannot be evaluated using traditional annual metrics alone. Performance needs to be tracked continuously, with a focus on customer behavior over time.
- Customer Lifetime Value (LTV): Measures the total value a customer generates over their full subscription period. This should factor in premium collected, claims cost, servicing cost, and retention duration. A strong model ensures LTV consistently exceeds acquisition and servicing costs.
- Monthly Churn Rate: Tracks the percentage of customers who cancel each month. Even small increases in churn can significantly reduce profitability, especially if acquisition costs are high.
- Average Subscription Duration: Indicates how long customers typically stay active. Longer durations improve profitability by spreading acquisition and onboarding costs over time. It also signals whether the product is delivering sustained value.
- Loss Ratio by Customer Cohort: Instead of looking only at overall loss ratios, insurers should track performance by customer groups (e.g., new vs retained customers, plan tiers, acquisition channels). This helps identify where risk or pricing issues are concentrated.
- Revenue Stability (Monthly Premium Consistency): Measures how predictable monthly income is across the portfolio. High volatility may indicate pricing gaps, churn issues, or overexposure to short-term customers.
- Plan Mix and Upgrade/Downgrade Trends: Tracks how customers move between pricing tiers. This helps insurers understand whether higher-value plans are being adopted and where revenue leakage may occur.
Operational Model Requirements for Subscription Insurance
Subscription auto insurance may feel simple to the customer, but it creates a more demanding operating model for the insurer.
Traditional auto insurance follows a fixed sequence: quote, bind, issue, then renew at the end of the policy term. Subscription models work differently. They run on a continuous lifecycle, where coverage is renewed monthly and customers may change plans, vehicles, or service levels far more often.
That means insurers cannot rely on operations designed for static policy administration. They need processes built for ongoing change.
Core Operational Capabilities
To run this model effectively, insurers need a few capabilities in place.
- Recurring billing and invoicing: The system must support monthly collections, payment retries, and proration when customers make changes mid-cycle.
- Rolling policy lifecycle management: Coverage needs to be managed as an active, ongoing service rather than a policy that only changes at renewal.
- Fast activation and deactivation: Customers expect coverage to start, stop, or switch quickly, without manual delays or back-office bottlenecks.
- Mid-cycle change handling: Operations must support vehicle swaps, plan upgrades, downgrades, and coverage edits at any point in the subscription period.
- Customer self-service support: Policyholders should be able to manage payments, plan changes, and account updates through digital channels without depending on manual support for every request.
Key Operational Risk Areas
The flexibility that makes subscription insurance attractive also creates operational pressure.
- Billing failures can disrupt active coverage: A missed or failed payment is not just a finance issue. If not handled properly, it can create coverage gaps, customer disputes, and compliance concerns.
- High churn increases processing volume: Frequent onboarding, offboarding, and account changes raise operational workload and can quickly strain teams that are still built around annual policy cycles.
- Bundled services increase coordination risk: When insurance is packaged with vehicle access, maintenance, or roadside services, multiple systems and partners must remain synchronized. If they do not, customer experience and margin control both suffer.
Technology Requirements for Subscription Auto Insurance
Subscription auto insurance cannot run effectively on traditional policy systems alone. The model depends on continuous updates, recurring billing, and real-time flexibility, which most legacy systems are not designed to handle.
To support this, insurers need a technology stack that enables ongoing policy orchestration, not just one-time policy issuance.
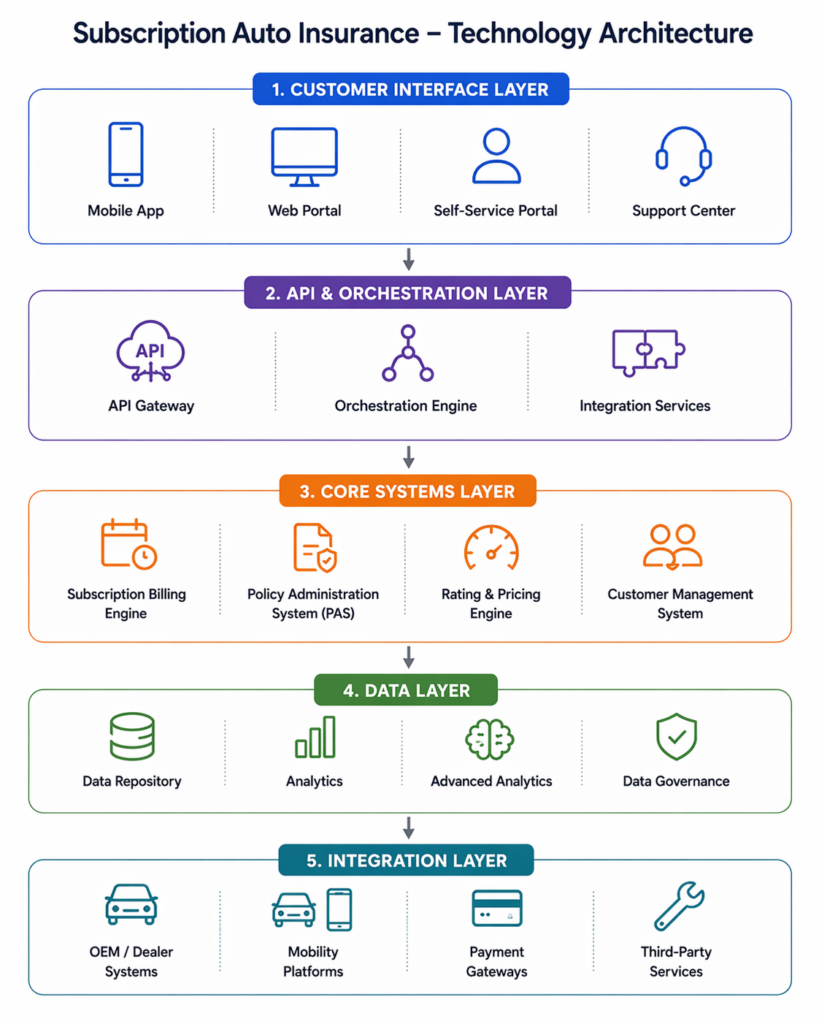
Core Technology Capabilities
To build and scale a subscription model, insurers should focus on these key components:
- Policy systems that support incremental updates:Policy administration system should allow vehicle swaps, plan changes, and coverage edits without requiring full re-issuance or manual intervention. Systems built only for fixed-term policies will struggle with this level of change.
- Billing systems designed for continuous adjustments: Monthly billing alone is not enough. The system must handle proration, failed payments, retries, and mid-cycle changes accurately and consistently at scale.
- Pricing engines that respond to event-based triggers: Rating logic should be able to update pricing when customers make changes, not just at quote or renewal. This includes plan upgrades, vehicle changes, and coverage modifications.
- Integration layers that support real-time coordination: If the product connects with OEM platforms, mobility providers, or third-party services, integrations need to be API-first and responsive. Delays between systems can create billing mismatches and poor customer experience.
- Customer platforms that enable self-service: Customers should be able to manage subscriptions, payments, and changes without manual support. This requires tightly connected front-end and core systems.
- Data systems that track behavior over time: Subscription models require visibility into churn, plan movement, and cohort performance. Data systems need to support continuous tracking, not just periodic reporting.
Integration Requirements
Subscription auto insurance rarely operates as a standalone system. In many cases, it sits inside a broader mobility ecosystem, which means insurers need strong integration across both internal and external platforms.
At a minimum, the technology stack should connect with:
- vehicle subscription platforms
- OEM and dealer systems
- mobility or ride-sharing applications
- payment gateways and billing providers
These integrations are essential for keeping pricing, billing, policy changes, and customer experience aligned across the full journey. If systems do not stay synchronized, even a well-designed product can create friction for both the insurer and the customer.
Related Read: How to Build Right Core Technology Stack for P&C Insurer in the USA
How Underwriting Changes in Subscription Auto Insurance
Underwriting in subscription auto insurance needs to work in a more dynamic environment, where coverage may change more often and customer relationships may be shorter or less stable over time. Instead of relying mainly on fixed-term assumptions, insurers need underwriting rules that can support ongoing adjustments while still protecting portfolio quality.
In practice, the biggest changes show up in a few areas:
- Eligibility needs to be tighter upfront: Clear rules are needed for which driver profiles, vehicle types, and coverage combinations are suitable. This prevents high-variability risks from entering a model designed for speed and flexibility.
- Re-rating becomes more event-driven: Pricing and underwriting should be reassessed when key changes occur, such as vehicle swaps, plan upgrades, or coverage edits. Trigger-based logic helps manage these changes without slowing down the experience.
- Shorter exposure periods need closer monitoring: Profitability can shift faster when customers stay for shorter durations. For example, a customer subscribing for one month and filing a claim early in the cycle can significantly impact margins.
- Entry and exit behavior matters more: Customers may activate coverage during high-usage periods and cancel afterward. Monitoring these patterns is critical to avoid adverse selection.
- Portfolio monitoring becomes more important: Underwriting needs to track performance by cohort, plan type, segment, vehicle category, and subscription duration to identify weak patterns early and adjust rules accordingly.
The key change is that underwriting becomes less about one-time risk assessment and more about managing risk across a product that is designed to stay flexible.
How Claims Management Needs to Change in Subscription Auto Insurance
Claims management in a subscription model needs to be built for speed, continuity, and coordination, not just settlement. Because customers can enter, exit, or modify coverage more frequently, the claims function has to operate in a way that support a model with frequent policy updates and shorter customer lifecycles.
In practical terms, insurers should focus on the following changes:
- Faster FNOL and intake workflows: Claims reporting should be instant and digital-first, with minimal steps. This reduces friction at the most critical moment and aligns with the overall subscription experience.
- Early-stage claim tracking and controls: Claims occurring soon after activation should be monitored closely, as they have a higher impact on profitability. This requires better visibility into claim timing relative to subscription start.
- Integrated service workflows: Claims systems need to connect directly with repair networks, roadside assistance, and service partners. This ensures faster resolution and avoids delays caused by disconnected processes.
- Real-time status and communication: Customers should be able to track claim progress, upload documents, and receive updates digitally. Lack of visibility can quickly impact satisfaction and retention.
- Cohort-based claims analysis: Instead of only tracking overall claims performance, insurers should analyze claims by plan type, vehicle category, acquisition channel, and subscription duration to identify patterns early.
- Flexible claims handling rules: The system should support policy changes during the claims lifecycle, such as plan upgrades or cancellations, without creating operational conflicts or manual intervention.
The key shift is that claims management needs to move from a linear, process-driven function to a more connected, real-time service layer that supports both operational efficiency and customer experience.
Regulatory Considerations for Subscription Auto Insurance
Subscription auto insurance introduces flexibility on the product side, but regulatory frameworks are still largely built around fixed-term policies. That creates a gap insurers need to manage carefully when designing and launching this model.
The goal is not just compliance, but ensuring that flexibility does not create regulatory risk, filing delays, or approval challenges across states.
Key Areas Insurers Need to Address
- Monthly renewal structure: Regulators may require clarity on how continuous monthly renewals are defined, whether they are treated as new policies, extensions, or a rolling contract. This impacts filings, disclosures, and compliance obligations.
- Cancellation and notice requirements: Even if the product allows easy cancellation, insurers must still comply with state-specific notice periods, non-renewal rules, and consumer protection requirements.
- Minimum coverage duration rules: Some jurisdictions may not fully support very short-term or highly flexible coverage structures. Insurers need to ensure the product aligns with minimum term expectations where applicable.
- Disclosure for bundled offerings: When insurance is packaged with vehicle access or other services, regulators may require clear separation and disclosure of:
- insurance vs non-insurance components
- pricing breakdown
- coverage terms and conditions - Filing and approval complexity: Subscription models often involve new pricing structures, billing logic, and product definitions. This can lead to:
- more detailed filings
- higher likelihood of objections
- longer approval timelines
Customer Strategy for Subscription Auto Insurance
Subscription auto insurance requires a different approach to customer strategy. Success depends not just on who you target, but on how the product fits into changing mobility needs and how clearly that value is delivered over time.
The model works best with customers whose mobility patterns are variable rather than fixed, and who are open to managing coverage as part of an ongoing service.
Target Segments to Focus On
Insurers should prioritize segments where variability in usage creates a natural fit:
- Urban and semi-urban drivers: More likely to have inconsistent driving patterns and changing vehicle needs
- Younger, digitally comfortable users: More open to managing products through apps and recurring payment models
- Subscription-oriented consumers: Already familiar with managing services through monthly payments
- Users of car subscription or leasing platforms: More likely to adopt bundled offerings where insurance is part of a broader package
- Convenience-driven, higher-income segments: Less price-sensitive and more focused on ease of management
How Insurers Should Approach Go-to-Market
Subscription auto insurance requires a different go-to-market approach compared to traditional policies.
- Embedded and partner-led distribution is a strong fit: The model aligns naturally with OEM platforms, vehicle subscription providers, and mobility ecosystems where insurance can be offered as part of a broader service
- Direct-to-consumer works when the product is simple: Clear pricing tiers and minimal configuration are critical for direct channels
- Acquisition should focus beyond price: Customers evaluate onboarding experience, billing clarity, and ease of use, not just premium levels
What Drives Customer Adoption in This Model
Adoption depends on how clearly the product fits into real usage and expectations:
- Clarity in what is included vs excluded: Customers need a clear understanding of what the monthly price covers, especially in bundled offerings
- Confidence in making changes without penalty: The ability to switch plans or vehicles without unexpected costs builds trust
- Consistency across the lifecycle: The experience from onboarding to claims should feel aligned, not fragmented
- Perceived control over the product: Customers should feel they can adjust coverage as their needs change without added complexity
Why Retention Matters More Than Acquisition
In this model, long-term value is driven more by how long customers stay than how many are acquired.
Insurers should actively manage:
- early churn, especially in the first few months
- engagement through ongoing interaction points
- clear pathways for plan upgrades or transitions
- service quality across claims and support
A customer who stays longer contributes significantly more value than one who frequently enters and exits.
When Subscription Auto Insurance Makes Sense for P&C Insurer
Subscription auto insurance is not the right fit for every insurer or every market. Before building it, insurers should assess whether the model aligns with their customer base, product design, operating model, and technology capabilities.
Decision Framework for Insurers
| Decision Area | What to Assess | Strong Fit Indicators | Warning Signs |
|---|---|---|---|
| Market fit | Whether customer demand supports a flexible monthly model | Urban or hybrid-driving markets, digital-first users, demand for convenience and lower commitment | Customers still prefer fixed annual policies and traditional billing |
| Product fit | Whether the product can be simplified into a recurring subscription structure | Standardized coverage tiers, simple monthly packaging, bundling potential | Highly customized products, complex rating structures, niche underwriting needs |
| Operational readiness | Whether internal teams can support frequent changes and continuous servicing | Ability to handle monthly billing, mid-cycle changes, fast activation, and self-service support | Heavy manual processing, slow servicing workflows, limited billing flexibility |
| Technology readiness | Whether core systems can support a subscription-based model | Modular PAS, recurring billing, real-time pricing, API integrations | Legacy systems built around fixed terms, batch processing, and limited integration |
| Regulatory fit | Whether the product can work within state-specific compliance requirements | Clear filing path, manageable disclosure needs, flexibility within target states | Unclear treatment of rolling renewals, strict cancellation rules, complex filing risk |
This model makes the most sense when there is alignment across all five areas. If one or two areas are weak, insurers may still explore the concept, but the launch path will likely be slower and more complex.
Strategic Takeaway
Subscription auto insurance is not just a product innovation. It is a business model decision. The stronger the fit across market demand, product structure, operations, technology, and compliance, the more realistic the opportunity becomes.
Conclusion
Subscription auto insurance is not just a different way to structure pricing. It requires insurers to rethink how products are designed, priced, operated, and supported across the full lifecycle.
For insurers exploring this model, the challenge is not whether the concept works. The real challenge is whether the organization is ready to support the coordination it requires across pricing, operations, technology, underwriting, and compliance.
Insurers need a structured approach to assess where the model fits, what capabilities need to change, and how to build it in a way that can scale without creating operational friction.
Insurance strategic consultants such as Practo Insura help insurers define the right model, align internal capabilities, and build the foundation needed to support subscription auto insurance effectively.
In the end, subscription auto insurance will not be defined by how innovative it looks on the surface. It will be defined by how well it is designed and executed behind the scenes
What Is Pay How You Drive Auto Insurance? How U.S. P&C Insurers Can Implement It.
Auto insurance pricing is already moving beyond fixed assumptions. Over the last few years, models like Pay As You Go (PAYG) have shifted pricing closer to real usage by asking a simple question: how much does someone drive?
Pay How You Drive (PHYD) takes that one step further. Instead of focusing only on mileage, it looks at something more telling, how that mileage is actually driven.
At its core, PHYD is a behavior-based insurance model where premiums are influenced by real driving patterns captured through telematics. Rather than relying primarily on traditional rating factors like age, ZIP code, or historical proxies, insurers begin to incorporate observed driving behavior into pricing decisions.
According to research, insurers using behavioral pricing models can improve risk segmentation accuracy by up to 30%.
This changes the role of data in underwriting. Instead of estimating risk upfront and leaving it largely static, PHYD allows insurers to continuously refine their view of risk based on how a policyholder actually behaves on the road.
Understanding the Pay How You Drive Insurance
PHYD is a behavior-based pricing model.
Premiums are adjusted based on continuous assessment of driving quality, not just miles accumulated. The insurer collects granular telematics data, processes it through a behavioral scoring engine, and applies a score-derived modifier to the base premium.
The key distinction from PAYG is that PHYD is not an exposure correction. It is a risk quality correction.
How Pay How You Drive Insurance Works
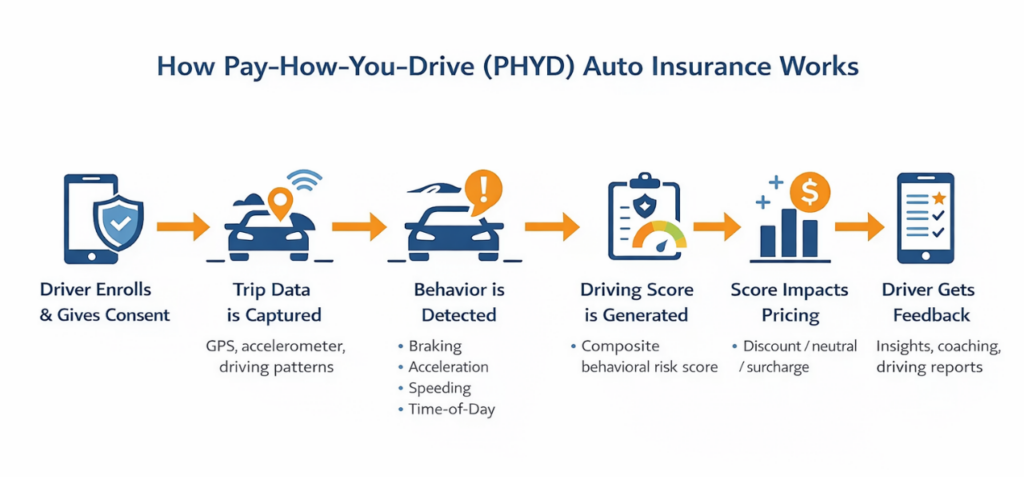
While the underlying technology can be complex, the customer and insurer journey typically follows a clear sequence:
- Enrollment and Consent: The policyholder opts into the program, agreeing to share telematics data through a mobile app, device, or connected vehicle system.
- Trip Data Collection: Each trip is recorded using sensors such as GPS and accelerometers, capturing movement, speed, and driving patterns.
- Behavioral Event Detection: The system identifies specific driving events, for example, hard braking, rapid acceleration, speeding, or late-night driving.
- Score Generation: These events are processed into a composite driving score, reflecting the overall risk profile of the driver.
- Pricing Adjustment: The score is translated into a pricing outcome, typically a discount, neutral adjustment, or surcharge, applied at renewal or, in some cases, during the policy term.
- Feedback Loop: Drivers receive insights or summaries of their driving behavior, creating a continuous feedback cycle between behavior and pricing.
This structured flow is what differentiates PHYD from simpler usage-based models. It is not just tracking activity, it is interpreting behavior and linking it directly to risk.
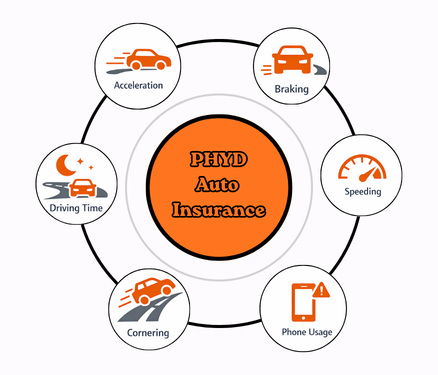
Behavioral Signals That Drive the Score in PHYD
The variables most predictive of loss frequency and severity are:
- Hard braking events: the strongest single predictor of loss frequency
- Rapid acceleration: correlated with aggressive driving patterns
- Speeding above posted limits: primary severity driver
- Time-of-day driving concentration: elevated risk in nighttime hours
- Phone distraction proxies: screen-state + motion fusion signals
Pricing Architecture & Behavioral Scoring for Pay How You Drive Auto Insurance
If PHYD changes how risk is observed, pricing architecture is where that insight turns into measurable financial impact.
At a structural level, PHYD does not replace traditional ratings. Instead, it layers behavioral intelligence on top of it, allowing insurers to refine pricing based on how risk is expressed over time, not just how it is assumed at policy inception.
This creates a dual-layer model where traditional underwriting establishes the baseline, and behavioral scoring adjusts that baseline dynamically.
Types of Pricing Structure in PHYD
Most PHYD programs follow a consistent structure:
- Base Premium: Calculated using traditional rating variables such as vehicle, coverage, territory, and driver history.
- Behavioral Modifier: A percentage-based adjustment applied on top of the base premium, reflecting observed driving quality over a defined scoring window.
In practice, this means two drivers with identical starting profiles may diverge over time based on how they actually drive. Pricing becomes less about assumed risk and more about continuously observed behavior.
Discount vs. Surcharge Design
The pricing design in PHYD is not just about adjustment, it’s about how risk is introduced into the product over time.
Most insurers begin with a discount-only model, where safer driving leads to lower premiums, but risky behavior does not immediately result in penalties. This reduces customer resistance and simplifies regulatory approval.
As data maturity improves, insurers shift toward bidirectional pricing, introducing both discounts and surcharges. This allows pricing to better reflect actual risk and helps maintain loss ratio discipline, especially for consistently high-risk drivers.
In-Term vs. Renewal Adjustment
Another core design choice is when behavioral data impacts pricing.
In renewal-based models, pricing is updated at the start of each policy term using past driving data. This approach is stable and easier to operate but slower to reflect behavior changes.
In in-term models, pricing adjusts during the policy period based on ongoing data. This improves accuracy but requires real-time billing capability and clear communication to avoid customer confusion.
Behavioral Variables & Pricing Impact on Insurance Premiums
Behavioral scoring is built on telematics-derived variables that demonstrate measurable relationships with loss outcomes. Each variable must be carefully selected, validated, and weighted based on its predictive strength.
| Variable | Measurement Method | Pricing Impact | Primary Data Source |
|---|---|---|---|
| Hard braking | Accelerometer - G-force threshold breach | High - strong loss frequency predictor | Mobile SDK / OBD-II |
| Rapid acceleration | Accelerometer + GPS speed change | Moderate-High | Mobile SDK / OBD-II |
| Speeding | GPS speed vs. posted limits (map-integrated) | High - linked to severity and frequency | GPS + map layer |
| Time-of-day driving | Trip timestamp segmentation (e.g., night driving) | Moderate -elevated risk periods | Mobile app / OEM feed |
| Phone distraction | Device sensor + screen interaction patterns | High - proxy for distracted driving | Mobile SDK |
| Cornering / handling | Gyroscope + accelerometer data | Moderate | Mobile SDK / OBD-II |
| Behavioral consistency | Pattern stability across trips | Low–Moderate | Scoring engine |
Not all variables carry equal weight. Insurers typically prioritize those with stable and statistically credible relationships to loss frequency, while continuously evaluating emerging signals such as distraction.
Score Translation to Pricing Bands
Once behavioral data is captured, it must be translated into a usable pricing signal.
Most PHYD programs aggregate individual variables into a normalized composite score, often on a 0-100 scale. This score is then mapped into pricing bands such as 'Excellent', 'Good', 'Fair' & 'High-Risk'.
These bands determine the final premium adjustment applied to the policy.
Typical structures include:
- Discount Corridor: ~5% to 30% reduction for better-than-average drivers
- Surcharge Bands: Applied to consistently high-risk behavioral profiles, where actuarially supported and regulatorily approved
Transparency vs. Black-Box Scoring
A critical design choice lies in how scores are presented:
- Transparent Models: Clearly indicate which behaviors influenced the score. This improves customer understanding, supports coaching, and reduces disputes.
- Black-Box Models: Rely on opaque machine learning outputs with limited explainability. While potentially more predictive, they introduce challenges in customer communication and are increasingly scrutinized by regulators.
In practice, most insurers move toward explainable scoring frameworks, balancing predictive accuracy with regulatory defensibility and customer trust.
Actuarial Validation Layer
For PHYD to function as a rating mechanism, not just a data feature & behavioral variables must meet actuarial standards.
Each variable entering the rating engine must demonstrate:
- A statistically credible relationship with loss frequency and, where relevant, loss severity.
- Sufficient data maturity, typically requiring 18-24 months of matched telematics and claims data.
- Stability across different driver segments and geographies.
Interaction Effects & Fairness Testing
Behavioral variables do not exist in isolation. They must be evaluated in the context of traditional rating factors.
For example:
- A speeding variable may correlate strongly with certain territories.
- Time-of-day driving may align with specific demographic patterns.
These relationships can introduce:
- Redundancy in rating factors
- Potential proxy effects for protected classes
As a result, actuarial validation must include:
- Interaction testing with existing rating variables
- Disparate impact analysis
- Documentation for regulatory filings
Operational Consideration: Pricing Stability
Beyond statistical accuracy, PHYD pricing models must also account for customer experience and retention.
Highly volatile pricing, driven by short-term behavioral fluctuations, can create confusion and dissatisfaction. Most insurers address this by:
- Using rolling averages or smoothing techniques
- Applying minimum data thresholds before score updates
- Limiting the frequency of pricing changes
This ensures that pricing remains both responsive and stable, balancing actuarial precision with real-world usability.
Technology & Data Infrastructure Required for Pay How You Drive Insurance Model
PHYD is not just a pricing model, it is a data-driven operating framework. Every pricing decision depends on how accurately driving behavior is captured, processed, and translated into risk signals.
In practice, successful PHYD programs are built on a layered architecture, where each layer plays a critical role in ensuring that raw telematics data becomes reliable, explainable, and usable for pricing.
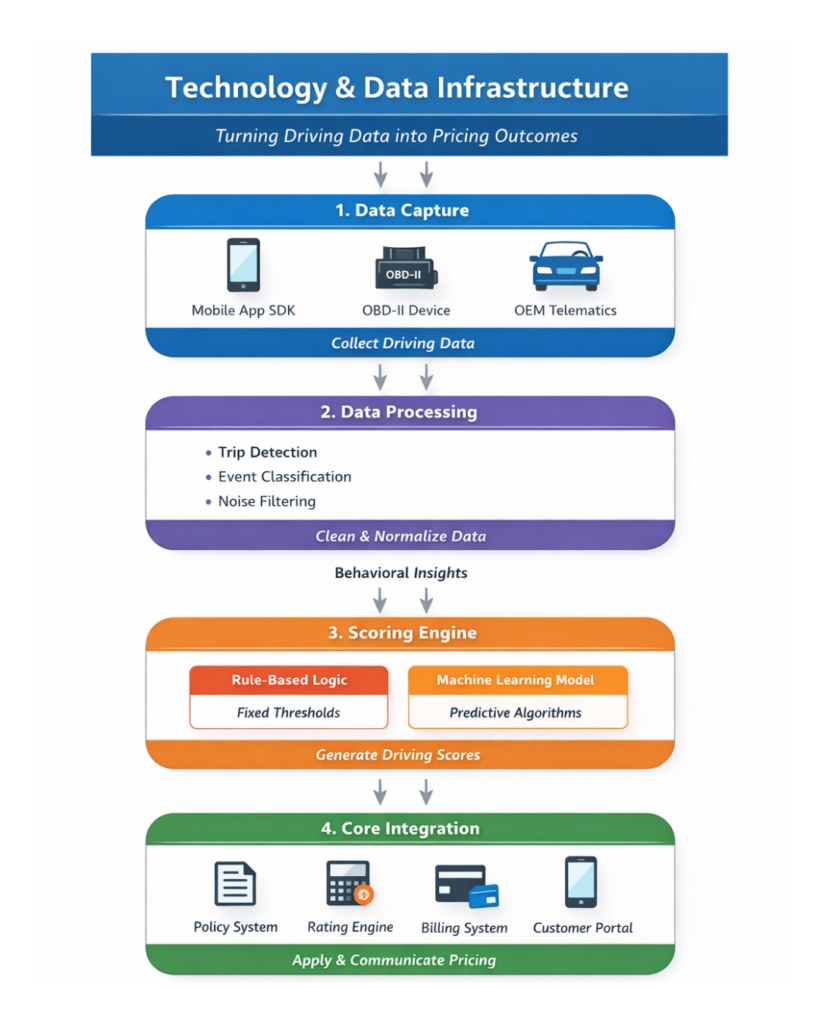
1. Data Capture Layer
The data capture layer defines what behavioral signals are available to the insurer. Each collection method comes with its own trade-offs between accuracy, cost, and scalability.
A. Mobile Application SDK
- Highest deployment flexibility, no additional hardware required.
- Requires explicit customer consent, battery optimization, and platform calibration (iOS vs. Android behavior differs).
- Captures inputs such as GPS, accelerometer, gyroscope, and screen interaction.
- Supports distraction detection through device usage patterns.
In most cases, this is the default starting point for PHYD programs due to ease of rollout and scalability.
B. OBD-II Dongle
- Provides consistent data quality through vehicle diagnostics (CAN bus integration).
- Strong signal accuracy for acceleration and braking events.
- Requires operational workflows for device shipping, activation, and returns.
- Limited capability for detecting phone distraction.
Suitable for programs prioritizing data precision over convenience, but with higher operational overhead.
C. OEM Embedded Telematics
- Most accurate and consistent data, as sensors are factory-installed.
- No additional effort required from the driver once enabled.
- Limited to newer connected vehicles.
- Data access depends on OEM partnerships and licensing agreements.
Increasingly important as connected vehicle adoption grows, especially for long-term strategic PHYD models.
2. Processing Layer
Raw telematics data cannot be used directly. The processing layer ensures that collected data accurately reflects real driving behavior.
This layer performs three critical functions:
- Trip Detection: Identifies the start and end of journeys, while filtering out stationary periods and non-driving movement.
- Event Classification: Categorizes events such as hard braking, speeding, or phone usage based on calibrated thresholds.
- Noise Filtering: Removes false positives caused by speed bumps, signal loss, or sensor inconsistencies.
Data quality at this stage directly impacts everything downstream. If trips are misclassified or thresholds are poorly calibrated, the behavioral signal becomes unreliable, affecting both scoring accuracy and pricing outcomes.
Because of this, the processing layer requires continuous monitoring and calibration, not just a one-time setup.
3. Scoring Engine
Once data is processed, it is translated into behavioral risk insights through the scoring engine. This is where insurers define how driving behavior influences pricing.
Rule-Based Scoring
- Uses predefined thresholds (e.g., braking beyond a certain G-force classified as harsh braking).
- Easier to implement and explain.
- Preferred in early-stage programs and regulatory filings.
Best suited for transparency, speed to market, and compliance clarity
Machine Learning Models
- Learn patterns from historical driving and claims data.
- Capture non-linear relationships between behavioral variables.
- Continuously refine scoring logic as more data becomes available.
Require:
- Larger datasets
- Model validation processes
- Explainability frameworks for regulatory acceptance
Model Governance Requirements
Regardless of scoring approach, governance is critical.
Key requirements include:
- Defined model retraining schedules (e.g., quarterly or based on meaningful data growth).
- Holdout testing against actual loss outcomes to validate predictive performance.
- Fairness testing to detect bias across demographic proxies.
- Version control and audit trails for regulatory review and filing support.
Without governance, even highly predictive models become difficult to justify in a regulated environment.
4. Core Integration Layer
Behavioral insights only create value when they are connected to core insurance systems.
This layer integrates telematics outputs into:
- Policy Administration System (PAS) → applies behavioral modifiers.
- Rating Engine → calculates final premiums.
- Billing Systems → supports renewal or in-term adjustments.
- Customer Interfaces (apps/portals) → provide feedback and transparency.
Without this integration, PHYD remains a disconnected data initiative rather than a functioning insurance product.
Why This Architecture Matters
Each layer builds on the previous one:
Data Capture → Processing → Scoring → Pricing Integration
A weakness in any layer, whether poor data quality, incorrect event classification, or weak integration can directly impact:
- Pricing accuracy
- Customer trust
- Regulatory compliance
For insurers, the goal is not simply to collect telematics data but to create a system where Behavior → Insight → Pricing → Feedback operates as a continuous, reliable loop.
Related Read: Top 7 Usage-Based Insurance Trends in the USA & How Auto Insurers Can Make the Shift
How Underwriting Changes in PHYD Auto Insurance
PHYD changes underwriting from a static, point-in-time assessment into a continuous, behavior-informed process.
In traditional auto insurance, underwriting decisions are made at policy inception using proxy variables, age, location, vehicle type, and prior history. In PHYD, these still matter, but they are no longer the full picture.
Risk is no longer just predicted upfront, it is observed and updated over time.
1. Shift from Static to Dynamic Risk Assessment
In a PHYD model, underwriting does not end at bind. Instead, it evolves throughout the policy lifecycle.
This creates two layers of risk evaluation:
- Initial Risk Selection: Based on traditional underwriting variables at quote and bind.
- Ongoing Behavioral Validation: Based on how the insured actually drives after the policy becomes active.
This shift allows insurers to move closer to true risk alignment, where pricing and underwriting decisions reflect real-world exposure rather than assumptions.
2. Role of Telematics in Risk Segmentation
Behavioral data introduces a new dimension to segmentation.
Instead of grouping drivers only by demographic or historical proxies, insurers can segment based on:
- Driving smoothness (braking, acceleration patterns)
- Exposure context (time of day, trip patterns)
- Distraction indicators (device interaction while driving)
- Behavioral consistency over time
This enables more granular classification, where two drivers with similar traditional profiles can be placed into different risk tiers based on observed behavior.
3. Rules, Triggers, and Data Credibility for Underwriting
Many PHYD programs define clear underwriting triggers tied to behavioral signals. For example, consistently high-risk scores may prompt review, while improving scores may support better pricing treatment.
At the same time, insurers need to decide when behavioral data is credible enough to act on. Limited trip volume, incomplete data, or device inconsistency can distort underwriting decisions. That is why most programs set minimum credibility thresholds before telematics data influences underwriting action.
4. How to Manage Adverse Selection and Operational Balance
Because many PHYD programs begin as opt-in offerings, they can attract safer drivers first, creating participation bias in early results. Insurers often manage this by comparing telematics and non-telematics cohorts separately and keeping behavioral underwriting aligned with pricing and product rules.
The practical challenge is balance. Too many triggers and exceptions can make underwriting difficult to manage. Most insurers start with a small set of high-value behavioral rules and expand as data quality and operational confidence improve.
How Pay How You Drive Changes Claims Management
PHYD does not just impact pricing, it also changes how claims are validated, investigated, and resolved. According to a Deloitte study, telematics-supported claims can reduce fraud-related losses by 20–40%.
Telematics data introduces a new layer of evidence that helps insurers move from post-loss reconstruction to data-supported verification.
1. FNOL & Incident Context
At the time of First Notice of Loss (FNOL), telematics data can provide immediate context such as:
- Trip timing and location
- Speed and movement patterns before impact
- Driving conditions (e.g., time of day)
This allows insurers to triage claims faster and prioritize cases based on severity and complexity.
2. Event Validation & Liability Support
Behavioral and trip data can help validate whether:
- A trip was active at the time of loss
- The vehicle was in motion or stationary
- Driving behavior aligned with reported events
For example, braking patterns or sudden deceleration signals can support impact confirmation, while speed data can assist in liability assessment.
This does not replace investigation, but it adds an objective reference point.
3. Fraud Detection & Dispute Reduction
PHYD introduces structured data that can reduce ambiguity in claims.
It can help identify:
- Mismatches between reported and actual trip data
- Suspicious timing or location inconsistencies
- Repeated behavioral patterns linked to higher-risk claims
This improves fraud detection while also reducing unnecessary disputes in legitimate cases.
4. Claims Segmentation & Handling
With behavioral insights, insurers can better segment claims:
- Low-risk, well-documented incidents → faster processing
- High-risk or inconsistent cases → deeper investigation
This supports more efficient allocation of adjuster effort and improves overall claims cycle time.
Regulatory & Compliance Considerations Before Launching
PHYD is not just a pricing model, it is a regulatory and governance exercise from the start.
Because behavioral data affects premium, insurers must ensure that data collection, scoring logic, and pricing adjustments are all filed, explainable, and defensible under state rules.
1. Filing & Rating Approval
Behavioral factors used in pricing usually need actuarial support before they can be filed and approved. Insurers must show that the variables have a credible relationship to loss outcomes and clearly define how scores affect premium.
In stricter states, regulators may prefer discount-only structures first and may push back on complex or opaque scoring models.
2. Transparency, Privacy & Fairness
Insurers also need to explain:
- what data is collected
- how it affects pricing
- why a driver received a given score or adjustment
This makes explainable scoring more practical than black-box models.
At the same time, telematics programs must align with customer consent, privacy disclosures, and data retention rules. Behavioral variables should also be tested for disparate impact, proxy bias, and state-specific non-discrimination requirements.
3. Audit Readiness & State Variation
PHYD programs need clear audit trails, version control, and documentation for filings, objections, and model changes. Since regulatory expectations differ by state, rollout usually needs to happen state by state, not as a single national launch.
At its core, compliance in PHYD is about keeping behavior-based pricing fair, transparent, and regulator-ready.
Customer Target & Retention Strategy for Pay How You Drive Insurance
1. Target Segments
PHYD usually attracts drivers who believe they drive better than average and are open to sharing data in return for pricing benefits.
Common target segments include:
- Young drivers (18-26): often face higher base premiums and have more to gain from strong behavioral scores.
- Digitally engaged customers: more comfortable with app-based tracking and feedback.
- Safety-conscious drivers: more likely to respond well to behavior-based pricing
- Multi-vehicle households: offer a larger premium base and broader driving data over time.
2. Acquisition & Channel Enablement
At acquisition, the value proposition needs to be simple and concrete. Leading with behavioral language alone is usually less effective than leading with clear pricing benefits.
Approaches that work well include:
- Savings calculators to show possible discount ranges
- Agent enablement so agents can explain scoring, handle privacy questions, and set realistic expectations
- Clear digital messaging that frames PHYD as fairer pricing and driver control, not surveillance
Confusing program communication at enrollment is one of the biggest reasons customers drop out early.
3. Engagement Architecture
PHYD works best when score feedback becomes part of the customer experience, not just a hidden pricing input.
Strong programs usually offer:
- Trip or score dashboards
- Behavioral trend summaries over time
- Simple coaching insights
- Milestones or streak-based engagement features
The goal is to help customers feel they are improving, not just being monitored.
4. Retention Risks
Three common issues can drive churn in PHYD programs:
- Privacy fatigue - customers become uncomfortable with ongoing data collection.
- Score disputes - customers feel trips were misclassified or scoring was unfair.
- Surcharge churn - customers expecting discounts may leave if they receive a higher premium instead.
According to Capgemini research, around 40% of consumers cite data privacy as the biggest barrier to telematics adoption.
These risks are usually managed through clear communication, transparent scoring, defined dispute processes, and practical improvement pathways for customers near higher-risk bands.
Difference Between Pay-As-You-Need vs Pay-As-You-Go vs Pay-How-You Drive Insurance
To understand where PHYD fits, it helps to look at how it builds on earlier on-demand models:
- Pay As You Need (PAYN): Pricing is based on when coverage is active. It is primarily time-based and operational in nature.
- Pay As You Go (PAYG): Pricing is based on how much a driver uses the vehicle, typically measured in miles. It improves exposure accuracy but treats most miles similarly.
- Pay How You Drive (PHYD): Pricing is based on how well the vehicle is driven. It introduces behavioral scoring, allowing insurers to distinguish between drivers with similar usage but different risk profiles.
| Dimension | PAYN | PAYG | PHYD | Why It Matters |
|---|---|---|---|---|
| Pricing Basis | Time / session | Mileage | Behavior | PHYD prices risk quality, not just exposure volume |
| Data Required | On/off timestamps | GPS odometry | Full telematics stream | Sensor depth drives scoring accuracy |
| Underwriting Value | Exposure timing | Exposure volume | Risk selection + segmentation | PHYD targets both loss frequency and severity |
| Pricing Complexity | Low | Moderate | High | Scoring model + actuarial validation required |
| Regulatory Friction | Moderate | Moderate | High | Behavioral factors need state-level actuarial justification |
| Customer Engagement | Low | Low–Moderate | High | Score dashboards enable active behavior coaching |
| Technology Lift | Low | Moderate | Significant | Scoring engine + PAS integration mandatory |
Related Read: What Is Pay-As-You-Need Auto Insurance?
Related Read: What Is Pay-As-You-Go Auto Insurance?
Conclusion
PHYD is not just a telematics feature, it reflects a shift toward behaviour-driven insurance, where pricing and risk are continuously aligned with real-world driving.
The challenge is not defining the model but executing it end-to-end. PHYD touches pricing, underwriting, data infrastructure, customer experience, and compliance. If these elements are not aligned, the program risks becoming fragmented rather than scalable.
Successful insurers approach PHYD as a strategic transformation, not just a product add-on.
This is where insurance strategic consultant like Practo Insura help insurers design, implement, and scale PHYD programs across product strategy, pricing, infrastructure, and go-to-market execution.
As the industry evolves, PHYD is becoming less optional and more foundational. The real advantage lies in how effectively insurers can operate it.